Introduction
Mobile health applications – from patient-facing apps to clinical tools – are transforming how healthcare is delivered and experienced. Healthcare mobile apps empower patients to manage wellness and chronic conditions, while equipping providers with real-time data and decision support. According to a Research in JMIR Mhealth Uhealth: The rise of smartphones, wearables, and cloud connectivity has fueled an explosion of these apps: over 350,000 mobile health applications are available on app stores worldwide (about 250 new apps released daily). This article explores what mobile health applications are, their benefits for patients and professionals, real-world use cases (including some of the best healthcare mobile apps globally), challenges like adoption and privacy, emerging trends (AI, wearables, digital therapeutics), and strategic recommendations for healthtech startups and healthcare organizations.
Table of Contents
Key Takeaways
Empowered Patients: Healthcare mobile apps empower patients with on-demand access to health information and services, resulting in more engaged and proactive care experiences.
Greater Convenience: These apps streamline routine tasks like appointment scheduling, prescription refills, and health record access, saving patients time and improving convenience.
Beyond the Clinic: Telehealth features and remote monitoring capabilities extend care beyond the clinic, enabling timely interventions and better management of chronic conditions
Improved Adherence: By providing medication reminders and personalized tracking, mobile apps help patients adhere to treatment plans and stay on top of their health, leading to improved outcomes
Further Reading
Benefits of Mobile Apps in Healthcare
Mobile apps are delivering significant healthcare apps benefits for all stakeholders – improving patient outcomes, increasing efficiency for providers, and enabling new models of care. Authorities like the U.S. FDA emphasizes that digital health technologies (including mobile apps) offer opportunities to improve medical outcomes and system performance. Key benefits of mobile apps in healthcare include:
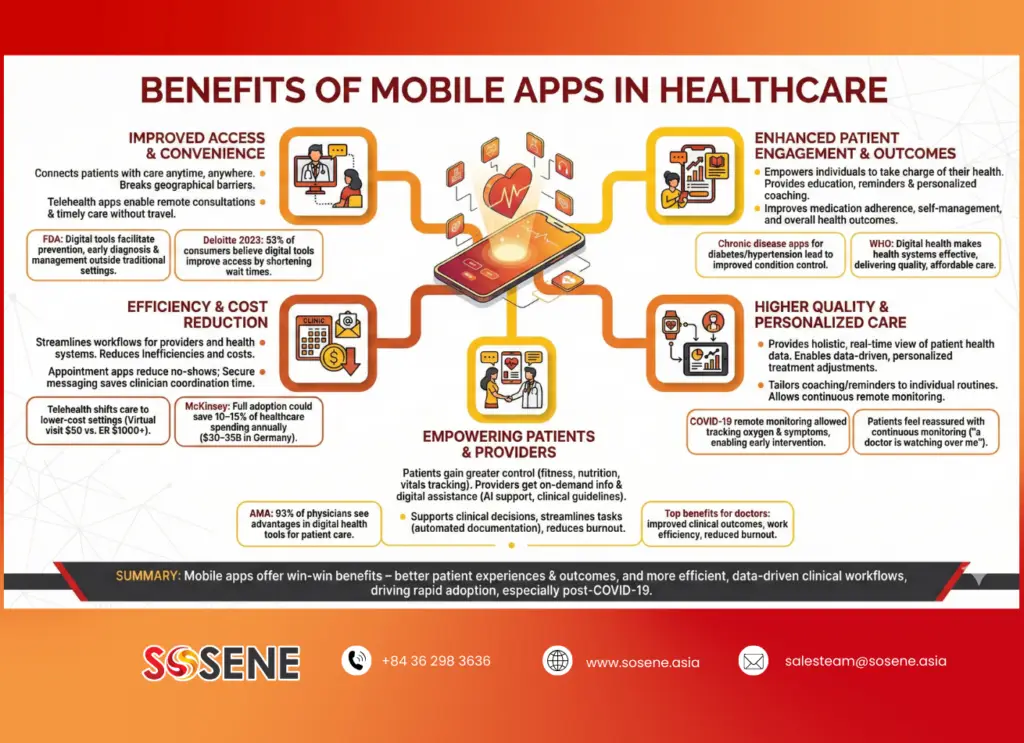
Improved Access and Convenience:
Mobile apps connect patients with care anytime, anywhere, breaking geographical barriers. Telehealth apps, for example, enable remote consultations so patients can receive timely care without travel.
According to the FDA, digital tools help “facilitate prevention, early diagnosis of life-threatening diseases, and management of chronic conditions outside traditional settings”. This increased access is also evident in consumer attitudes – in a Deloitte 2023 survey, 53% of consumers said digital tools (like AI in apps) could improve healthcare access by shortening wait times.
Enhanced Patient Engagement and Outcomes:
Healthcare mobile apps for patients empower individuals to take charge of their health. Apps can provide education, reminders, and personalized coaching that drive healthier behaviors and better adherence to treatments. Studies show mHealth interventions improve medication adherence, self-management, and overall health outcomes.
For instance, chronic disease apps for diabetes or hypertension allow patients to log readings and receive feedback, leading to improved control of those conditions. The World Health Organization notes that digital health can make health systems more effective and deliver quality, affordable care, ultimately improving population health outcomes.
Efficiency and Cost Reduction:
For providers and health systems, mobile apps and digital workflows create efficiencies that reduce inefficiencies and costs.
Simple examples are appointment-scheduling apps that reduce no-shows and optimize clinic flow, or secure messaging apps that save clinicians’ time on coordination. Telehealth apps shift care to lower-cost settings – a virtual visit ($50) instead of an ER visit ($1000+) yields immediate savings. At scale, these efficiencies add up: McKinsey analysis finds that fully adopting digital health (including mobile solutions) could save 10–15% of healthcare spending in many countries. In Germany, for example, this equates to $30–35 billion in annual savings for the health system. Such savings come from preventing complications via early intervention and shifting care from hospitals to home monitoring.
Higher Quality and Personalized Care:
Mobile apps can improve quality of care by giving providers a more holistic, real-time view of patient health data. Connected devices (like wearables) and symptom-tracking apps feed data to clinicians between visits, enabling data-driven, personalized treatment adjustments. Digital tools also help make medicine more personalized – for instance, apps can tailor coaching or medication reminders to an individual’s routine. This personalized approach can lead to better patient satisfaction and outcomes. In one example, remote monitoring apps for COVID-19 allowed doctors to track patients’ oxygen and symptoms multiple times a day, intervening early if readings worsened. Patients reported feeling reassured that “a doctor is watching over me” when using such apps at home. Overall, mobile health apps help increase care quality by facilitating continuous care and timely decision-making.
Empowering Patients and Providers:
Perhaps most importantly, mobile health tech empowers end users. Patients gain greater control over their health, with tools to track fitness, nutrition, medications, vital signs, and more. Providers are empowered with on-demand information and digital assistance (e.g. clinical guidelines apps or AI-driven diagnostic support).
In fact, an AMA survey found that 93% of physicians now see advantages in using digital health tools for patient care, up from 85% in 2016. Top reasons cited by doctors for embracing mobile and digital tools are improved clinical outcomes, work efficiency, and reduced burnout. By streamlining tasks (e.g. automated documentation, easy communication) and supporting clinical decisions, apps let clinicians focus more on patient care.
In summary, mobile apps in the healthcare industry offer win-win benefits – better patient experiences and outcomes, and more efficient, data-driven clinical workflows. These benefits have driven rapid growth in adoption, especially following the COVID-19 pandemic which proved the value of virtual care.
Mobile Apps for Patients: Empowering Personal Health Management
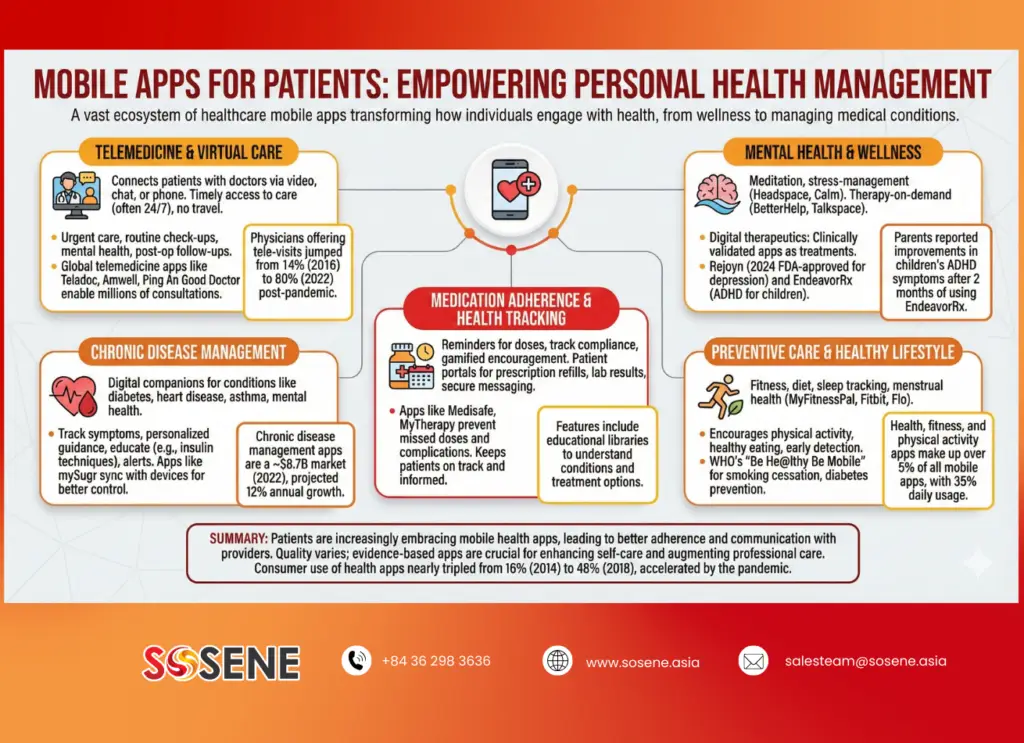
There is a vast ecosystem of healthcare mobile apps for patients, addressing needs from wellness and prevention to managing serious medical conditions. These patient-facing apps are transforming how individuals engage with healthcare on a daily basis. Key categories and use cases include:
Telemedicine and Virtual Care:
Telehealth apps connect patients with doctors via video calls, chat, or phone. Leading telemedicine apps like Teladoc, Amwell, or China’s Ping An Good Doctor have enabled millions of remote consultations worldwide.
During the pandemic, usage of virtual visit apps skyrocketed – the share of physicians offering tele-visits jumped from 14% in 2016 to 80% in 2022. Patients benefit from timely access to care (often 24/7) without needing to travel, which is particularly valuable for those in remote areas or with mobility issues. Telemedicine apps are used for urgent care, routine check-ups, mental health counseling, and even postoperative follow-ups. Mobile apps in healthcare industry settings are thus extending care beyond hospital walls, improving convenience and potentially outcomes (e.g. by enabling prompt treatment interventions).
Chronic Disease Management:
A large segment of mobile health apps in healthcare focuses on helping patients manage chronic illnesses like diabetes, heart disease, asthma, or mental health conditions. These apps serve as digital companions that track symptoms and deliver personalized guidance. For example, the app mySugr (developed in Europe) helps diabetes patients log blood sugar, insulin doses, and lifestyle data; it can sync with glucose monitors and insulin pens to provide feedback. Pharma companies Roche and Novo Nordisk even integrated mySugr with smart insulin delivery devices – enabling patients to automatically record doses and share data with providers (Deloitte). Such apps educate patients (e.g. proper insulin injection techniques, diet tips) and send alerts for out-of-range readings. The impact is significant: better day-to-day disease control and fewer acute exacerbations. In fact, disease management apps are a fast-growing market segment (worth ~$8.7B in 2022, projected 12% annual growth) as populations age and chronic conditions rise. Notably, obesity and mental health apps are among the largest sub-segments, reflecting global demand for lifestyle and psychological support via mobile platforms.
Medication Adherence and Health Tracking:
Forgetting to take meds or not following care plans are common issues that apps aim to solve. Medication reminder apps (like Medisafe or MyTherapy) send alerts for each dose and track compliance, often with gamified encouragement. Some allow family or caregivers to monitor adherence as well. There are also patient portal apps (often provided by hospitals or insurers) that enable prescription refill requests, viewing lab results, and secure messaging with doctors – all from a phone. According to Deloitte, common features of patient companion apps include “prescription refill reminders with remote ordering and delivery notifications” and educational libraries to help patients understand their condition and treatment options. By keeping patients on track and informed, these apps improve outcomes and reduce complications (e.g. preventing missed doses or duplicated therapies).
Mental Health and Wellness:
The mobile app revolution has extended to mental well-being. Meditation and stress-management apps (Headspace, Calm) have hundreds of millions of downloads globally. Therapy-on-demand apps (BetterHelp, Talkspace) connect users to licensed counselors via chat or video, lowering barriers to accessing mental health care. Notably, a new class of digital therapeutics has emerged for mental health: these are clinically validated apps that treat conditions.
For example, Rejoyn is an app recently approved (2024) by the FDA to help treat depression in patients with incomplete response to medication. It delivers a structured 6-week cognitive behavioral therapy program via smartphone, with exercises and mood tracking, effectively acting as a supplement to in-person therapy. Another example, EndeavorRx, is a prescription video-game-like app for children with ADHD that was FDA-cleared to improve attention through digital exercises. Parents reported improvements in kids’ symptoms after 2 months of use. These apps underscore how mobile health apps in healthcare are not just promoting wellness but can serve as treatments themselves – a paradigm called digital therapeutics.
Preventive Care and Healthy Lifestyle:
Many of the best healthcare mobile apps globally fall into the fitness and preventive care arena. Step counters, diet logs, sleep trackers and menstrual health apps (e.g. MyFitnessPal, Fitbit app, Flo) help users maintain a healthy lifestyle. While sometimes considered “wellness” rather than clinical, they have real healthcare impacts: encouraging physical activity, healthy eating, and early detection of issues. A post-pandemic analysis noted health, fitness and physical activity apps now make up over 5% of all mobile apps, with daily usage rates of 35% among those who download them (European Society Of Medicine). High engagement suggests these tools are fostering health awareness at scale. Some apps even integrate with national health campaigns – for example, the WHO’s “Be He@lthy Be Mobile” initiative leverages mobile programs for smoking cessation and diabetes prevention in multiple countries. Overall, these apps empower users to take preventive actions that can reduce the burden on healthcare systems long-term.
Patients are increasingly embracing mobile health apps across these use cases. Even before COVID-19, Accenture surveys showed consumer use of health apps nearly tripled from 16% in 2014 to 48% in 2018, and this trend accelerated with the pandemic. By managing appointments, vitals, medications, and even mental health through their smartphones, patients become more informed and engaged partners in care. As a result, providers see better adherence and communication. It’s important to note, however, that not all health apps are evidence-based – the quality varies widely. Thus, clinicians and organizations often curate recommended apps for patients (e.g. some health systems prescribe apps from an approved formulary). When well-designed and integrated, healthcare mobile apps for patients can significantly enhance self-care and augment professional care.
Mobile Apps for Healthcare Professionals: Enhancing Clinical Practice

Healthcare providers – physicians, nurses, and allied staff – have also rapidly adopted mobile apps and devices in their daily practice. Today’s clinicians are rarely found without a smartphone or tablet in hand, using them as indispensable medical tools. A few ways mobile apps for healthcare professionals are improving clinical workflows and patient care include:
Clinical Reference and Decision Support:
One of the earliest and most prevalent uses of mobile in medicine is quick access to medical references. Apps like UpToDate, Epocrates, or Medscape allow doctors to instantly look up drug information, dosing calculators, clinical guidelines, and disease literature at the point of care. According to a Wolters Kluwer survey, 72% of physicians access drug info on smartphones and over half use apps for clinical references or evidence-based tools during patient encounters. This on-demand knowledge helps ensure accurate prescribing and up-to-date care decisions. Many clinicians also use diagnostic aids – for instance, dermatoscopic image libraries for skin lesions or AI-driven symptom checker apps as a “second opinion” for complex cases. The benefits of mobile apps in healthcare here are better-informed providers and reduced errors, which translate to improved patient safety.
Communication and Collaboration:
Secure messaging and team collaboration apps have become vital in hospital settings. Instead of relying on pagers or phone tag, clinicians use apps like TigerConnect, WhatsApp (encrypted for health use), or proprietary hospital chat apps to communicate in real-time about patient care. A nurse can send a photo of a patient’s wound to a surgeon for consultation, or a doctor can notify a whole care team about new orders, all via a mobile interface. This instant communication accelerates decision-making and coordination. For example, a HIMSS survey found 44% of physicians regularly communicate with nurses/colleagues using smartphones. Replacing archaic workflows with modern messaging reduces delays and lengths of stay – one initiative with smartphone communication showed reduced ER admission times and faster nurse response in a hospital, improving overall efficiency. Moreover, mobile communication tools proved critical during COVID surges, enabling remote updates from isolation units and tele-rounding.
Electronic Health Records (EHR) on the Go:
Major EHR systems now offer mobile apps (e.g. Epic’s Haiku/Canto, Cerner’s PowerChart mobile) that let clinicians review charts, enter orders, and update documentation on a tablet or phone. This mobility means providers can manage patient care from anywhere – a physician can respond to a lab alert or refill request on their phone after hours, or input notes during a home health visit. It also means less time tied to a desktop, contributing to workflow flexibility and potentially reducing burnout. In a 2022 AMA study, physicians cited integration with EHR systems as a top requirement for any digital tool. When a mobile app seamlessly connects to the clinical record, it streamlines adoption since the app becomes an extension of existing workflows rather than an isolated gadget. Hospitals that deploy mobile EHR access see improved rounding efficiency and more timely order entry (e.g. orders placed during patient exams instead of waiting to find a workstation).
Remote Monitoring and Physician Dashboards:
As patients use more health apps and wearables, providers are leveraging companion interfaces to monitor patient-generated data. For example, a cardiologist might use a portal or app to review daily blood pressure or ECG readings uploaded from patients’ devices. During the pandemic, many practices set up remote patient monitoring (RPM) programs using mobile apps that patients interact with and that feed data back to clinicians. RPM apps for heart failure, diabetes, or COVID-19 send alerts to providers if readings are out of range, enabling proactive outreach. Doctors have grown more enthusiastic about such tools – 53% of physicians in 2022 showed strong enthusiasm for remote monitoring devices, a big jump from prior years. Mobile tech allows continuous care: instead of episodic check-ins, providers can virtually “round” on patients daily through data. This can lead to fewer hospital readmissions and better management of chronic conditions. A McKinsey review found remote monitoring of vital signs could save billions and was highly popular among doctors and patients involved in pilot programs.
Professional Training, CME and Scheduling:
Physicians and nurses also use general productivity and education apps. Many medical journals and CME (continuing education) providers have apps so clinicians can read the latest research or take CME quizzes on-the-go. Procedure simulation apps and even AR/VR tools on tablets help surgeons and trainees practice skills virtually. Additionally, scheduling apps help manage on-call rotations and shift swaps among hospital staff, improving workforce management. In telemedicine, special clinician-side apps allow doctors to conduct video visits or e-consults from their phone, adding flexibility to work location and hours.
Adoption of these mobile tools among healthcare professionals is now mainstream. Surveys show around 80–90% of physicians use smartphones for work purposes, and the average doctor uses almost 4 different digital tools in clinical practice (up from 2.2 tools in 2016). The attitude shift is remarkable – whereas a decade ago concerns about privacy, security, or liability slowed mobile uptake, today most providers recognize that thoughtfully designed apps enhance care delivery. Key requirements remain: physicians want reassurance of HIPAA-compliant security, reliable performance, EHR interoperability, and malpractice liability coverage when using apps. When these needs are met, clinicians are more than willing to integrate mobile health tech into their daily routine. The end result is mobile apps and healthcare providers working in tandem to deliver care more efficiently and effectively, whether at the bedside or through a screen.
Challenges in Adoption and Data Privacy Concerns
Despite the clear benefits, the proliferation of mobile health apps also brings challenges in adoption and data privacy that stakeholders must address. Some of the key concerns include:
- Data Security and Privacy Risks: Mobile health apps often handle highly sensitive personal health information (PHI), from medical history to real-time biometric data. This raises concerns about how securely apps store and transmit data. Unfortunately, many consumer health and wellness apps are not covered by strict healthcare privacy laws, and there have been alarming breaches of trust. A 2023 Duke University report found that data brokers were selling information identifying individuals by their mental health app data, including diagnoses, names, addresses, even ethnicities. This data had been “freely handed over” to seemingly benign wellness or therapy apps, only to be later aggregated and sold without users’ knowledge. Such revelations undermine public trust. If patients fear their intimate health details could be leaked or misused, they will be reluctant to use these apps or share data. Healthcare providers and IT departments also worry about privacy when integrating third-party apps – a compliance failure could violate regulations like HIPAA or GDPR (with hefty penalties). Ensuring robust encryption, anonymization, and transparent privacy policies is thus paramount for any mobile health solution.
- Lack of Regulation and Quality Control: The sheer number of health apps – 350k+ and growing – means quality varies widely. Unlike drugs or medical devices, most apps are not rigorously evaluated or regulated (except certain ones classified as medical devices). This leads to a “digital wild west” where some apps make unproven claims or have poor accuracy. For example, there may be dozens of diabetes apps, but only a few have clinical evidence backing their effectiveness. Navigating this space is challenging for both patients and clinicians – it’s hard to know which apps to trust. Regulatory bodies are catching up (the FDA has issued guidance on which apps qualify as regulated medical devices), and organizations like ORCHA and HIMSS evaluate apps against standards. Still, the current lax approach to data privacy and security in many mobile health apps highlights the need for stronger oversight. As health apps become more central to care, regulators will likely impose stricter rules to ensure safety and efficacy, similar to pharmaceuticals.
- Integration and Interoperability Issues: To fully realize the benefits, mobile apps should integrate with existing healthcare IT systems (EHRs, pharmacy systems, etc.) and with each other. Siloed apps that cannot share data create frustration and limit usefulness. For instance, if a patient’s glucometer app doesn’t send readings to the clinic’s record, the doctor might not act on that information. Many providers hesitate to adopt new apps because of workflow fragmentation – they don’t want to check multiple dashboards that don’t sync. Integration is getting better with standards like HL7 FHIR APIs, and some EHRs have app marketplaces, but achieving seamless interoperability is still a work in progress. Hospitals and startups need to prioritize integration during development/deployment.
- User Adoption and Behavior Change: Even when an app is well-designed, convincing people to use it consistently can be difficult. Mobile apps and healthcare workflows must be intuitive and truly solve a pain point, otherwise busy clinicians won’t incorporate them and patients will abandon them. Some challenges on this front:
- Digital Literacy: Not all patients (or providers) are tech-savvy. Elderly patients or those with low literacy might struggle with complex app interfaces. Solutions must account for usability across demographics (e.g. simple design, multi-language support, training).
- Workforce Resistance: Clinicians already face alert fatigue and heavy workloads. A new app that adds documentation or device management burdens can face pushback. Change management and demonstrating clear time-saving value are key to overcoming this.
- Trust and Efficacy: Clinicians may be skeptical of app-generated data reliability. Patients might not trust automated advice without physician reassurance. Building trust requires clinical validation and endorsements. It also takes time for culture to shift – e.g. initially some doctors feared telehealth would be inferior, but high satisfaction rates (74% of patients were satisfied with virtual care in an Accenture survey) overcame that.
- Privacy Regulations and Compliance: Healthcare organizations deploying apps have to ensure compliance with health privacy laws (HIPAA in the US, GDPR in Europe, etc.). This can be complex when apps involve cloud services or data crossing jurisdictions. Ensuring proper consent, data encryption, access controls, and audit trails is necessary but technically challenging, especially when integrating consumer-grade devices. There is also the question of data ownership – patients are generating data on their phone; when is it a part of the medical record? Who is responsible if that data is breached or misinterpreted? Hospitals must develop policies around mobile health data governance.
In summary, while mobile health apps hold great promise, stakeholders must navigate the challenges of adoption carefully. Addressing privacy and security up front is non-negotiable – both to protect users and to maintain trust in digital health innovations. Additionally, focusing on interoperability and user-centered design will help ensure these apps are actually used and useful. The good news is that clinicians and patients have shown willingness to adopt digital tools when they clearly improve care. As one physician leader noted, “validated digital health tools that improve health while streamlining burdens” are enthusiastically received – the onus is on developers and implementers to meet those standards.
Emerging Trends: AI, Wearables, and Digital Therapeutics

The landscape of mobile health is continually evolving. Emerging technologies are making healthcare mobile apps more intelligent, data-rich, and therapeutically powerful. Here aresome key trends shaping the future of mobile health apps:
Artificial Intelligence (AI) and Chatbots:
AI is increasingly being embedded in mobile health applications to provide personalized insights and automate tasks. For example, AI-driven symptom checker apps (like Ada, Buoy) can triage users by analyzing their inputs against vast medical databases – essentially providing an initial assessment before one sees a doctor. AI chatbots in therapy apps (e.g. Woebot, Wysa) converse with users to support mental health using cognitive-behavioral techniques. Early evidence suggests AI virtual health assistants can help manage chronic conditions by coaching patients daily. On the provider side, AI algorithms can analyze data from mobile devices (like heart rate trends, medication adherence) and alert clinicians to patterns of concern. Generative AI is also making inroads – from drafting clinical documentation after a patient visit to answering patients’ questions via an app chatbot. Notably, consumers are optimistic about AI in healthcare: over half (53%) of U.S. consumers believe generative AI will improve healthcare access and efficiency, according to a 2023 Deloitte survey. To leverage AI safely, developers must ensure algorithms are bias-checked and explanations are transparent, but the potential to scale personalized care with AI is immense.
Wearable Integration and Internet of Medical Things (IoMT):
The fusion of wearables with mobile apps is enabling continuous health monitoring. Modern smartwatches and fitness bands now include medical-grade sensors – for instance, the Apple Watch’s built-in ECG can detect atrial fibrillation and alert the user to seek care. In fact, the Apple Watch’s ECG feature (cleared by FDA in 2018) and its newer AFib History tracking have broken ground as digital health tools that cardiologists can utilize with patients. Other wearables like the Fitbit and Samsung Galaxy Watch also have FDA-cleared algorithms to passively screen for arrhythmias or track heart health Beyond heart metrics, wearable patches and smart rings measure everything from glucose levels (CGM devices) to blood pressure and sleep apnea events. Mobile apps act as the hub for these wearables, collecting data and often using AI to interpret it (e.g. detecting abnormal patterns).
The IoMT trend means a patient’s phone could continually receive data from multiple body-worn or home sensors – forming a “health dashboard” for both the individual and their clinicians. This real-time data flow enables truly preventive healthcare: apps can prompt a tele-consult when a reading goes out of range, or even automatically adjust an insulin pump via closed-loop systems. As 5G networks expand, expect faster and more reliable data syncing from wearables to cloud platforms, facilitating near real-time monitoring at scale. The challenge will be sifting through the data deluge – which again is where AI can help by highlighting only actionable signals.
Digital Therapeutics (DTx):
We are witnessing the rise of mobile apps that are the therapy. Digital therapeutics deliver clinical-grade interventions via software to prevent or treat diseases. They must undergo rigorous trials and regulatory approvals. Besides the earlier-mentioned mental health DTx (Rejoyn for depression, EndeavorRx for ADHD), there are apps like Insulia (for diabetes management), Nerivio (a smartphone-controlled wearable for migraine relief), and apps for substance use disorders (e.g. reSET-O for opioid addiction). These therapeutics often require a prescription and are sometimes reimbursable by insurance. The trend is expanding into areas like hypertension, insomnia, and chronic pain.
For healthcare providers and pharma companies, DTx opens a new modality to complement drugs – or even eventually replace certain medications with software-based treatment. An example is chronic insomnia: instead of prescribing a sedative, a doctor might prescribe a CBT-I therapy app like Somryst. Governments in some regions (Germany’s DiGA initiative) now have pathways to approve and cover digital health applications. For startups and developers, it means that investing in clinical evidence and regulatory compliance can pay off by unlocking payer reimbursement and clinician trust. Over the next few years, expect more “prescription apps” to emerge, creating an app formulary alongside pharmaceuticals. This will also necessitate updating medical training so clinicians know how to “dose” and monitor digital therapies.
Advanced Sensors and Remote Diagnostics:
Beyond typical wearables, innovations in biosensors are bringing lab-level diagnostics to smartphones. There are smartphone camera addons that can do an ECG or ultrasound, urine analysis strips that the phone camera can read, even apps using the phone’s microphone for respiratory diagnostics (e.g. detecting COPD exacerbation from cough sounds). AI combined with these sensors can potentially diagnose conditions early. For instance, the smartphone camera can detect blood oxygen or hemoglobin levels under certain lighting with algorithmic analysis – turning a regular phone into a basic medical tricorder. As these technologies mature, mobile apps will not just collect patient-reported data but perform automated health checks, some of which traditionally required clinic visits. Regulatory oversight will be crucial here to ensure accuracy and safety.
Personal Health Records & Ecosystems:
Tech giants are building ecosystems that aggregate health data for individuals. Apple’s Health app and Google Fit, for example, allow data from different apps and devices to be centralized on the phone. This gives patients a holistic view (steps, nutrition, labs, EHR records from connected hospitals) in one place and can be shared with providers. We’re moving toward a future where individuals carry a longitudinal personal health record on their phone. This can greatly improve care continuity – imagine a world where any clinician, with patient consent, can instantly review the patient’s complete history via a mobile device. Big tech firms are also exploring health “super apps” that integrate multiple services: e.g. WeChat in China has mini-programs for booking doctor appointments, paying bills, insurance, and telehealth all within one platform. Such integration simplifies the user experience and increases adoption.
Augmented Reality (AR) and Virtual Reality (VR):
AR/VR are niche but growing in healthcare mobile applications. AR apps on tablets are being used by surgeons for image-guided procedures (overlaying MRI images onto a patient during surgery). VR modules on mobile (with goggles) are used for pain distraction therapy (e.g. easing burn wound dressing pain) and for medical education/training simulations. As mobile processors and graphics improve, we could see more interactive 3D guides for patients too – for instance, an AR app to help patients visualize how to do physical therapy exercises correctly at home, or to overlay health information onto food labels for dietary guidance.
All these trends point to a future where mobile apps and healthcare are inextricably linked. The smartphone is becoming a health platform: it can sense, analyze, intervene, and communicate. The convergence of AI, sensors, and connectivity will make mobile apps even more integral to both acute and chronic care. Importantly, these technologies should not operate in isolation – integration into the healthcare system and maintaining the human touch in care remain crucial. As Deloitte’s 2024 outlook noted, the challenge is to harness these tools in ways that advance health equity and trust, not widen gaps. With thoughtful implementation, emerging tech can enhance personalization and reach underserved populations (for example, AI triage in apps could help areas with doctor shortages, and translated app interfaces can break language barriers). The coming years will be about scaling these innovations and proving their value in large populations.
Strategic Recommendations for Startups and Healthcare Organizations
For healthtech entrepreneurs, providers, and hospital IT leaders looking to build or deploy mobile health solutions, here are strategic recommendations to ensure success:
- Prioritize User-Centered Design and Engagement: The most effective healthcare apps are those that patients or clinicians want to use. Conduct thorough user research with your target audience (be it busy nurses or elderly patients) and co-design the app to fit naturally into their lives or workflows. Keep interfaces intuitive and accessible – e.g. large simple buttons for seniors, dark mode for doctors doing night shifts. Incorporate behavior change techniques (gamification, personalized nudges) to keep patients engaged over the long term. Remember that healthcare mobile apps compete with consumer apps for user attention – a polished user experience and clear value proposition are essential to avoid abandonment after the first try.
- Demonstrate Clinical Efficacy and Safety: Especially for startups, gaining the trust of healthcare providers and payers will require evidence. Invest in clinical validation early – pilot your app in a clinical setting, run a study or trial to show improved outcomes (e.g. better A1C control for a diabetes app, reduced rehospitalizations for a cardiac app). Collecting data on both outcomes and user satisfaction will give you the leverage to approach hospitals or insurers. If your app provides medical advice or therapy, consider pursuing regulatory clearance (FDA or equivalent) to stand out as a credible, safe solution. In a world of hundreds of thousands of apps, a strong evidence base will differentiate you as one of the best healthcare mobile apps truly making a difference.
- Ensure Privacy, Security, and Compliance: Embed privacy by design in your product. Use encryption for any stored or transmitted health data, employ robust user authentication, and be transparent about data use. For startups, getting HIPAA-compliant (or meeting GDPR requirements abroad) is a must if you handle identifiable health data – this may involve investing in secure cloud infrastructure and legal guidance. Perform regular security audits and have a plan for security updates. For healthcare provider organizations deploying apps, vet vendors thoroughly and ensure Business Associate Agreements are in place where needed. Given the heightened concerns around data privacy (with good reason, as shown by the Duke study on data brokers), making privacy a core feature (not an afterthought) will build user trust and protect your brand. Apple’s CEO famously said “privacy is a fundamental human right” – treating health data with that level of respect is key to user adoption.
- Integrate with Existing Systems and Standards: Silos won’t survive long in healthcare. If you’re a startup, design your app to integrate with popular EHRs or health APIs. Use standardized data formats (HL7 FHIR, SNOMED codes, etc.) so that your app’s data can easily plug into hospital IT systems. Seek partnerships with platform providers – for example, participating in Epic’s App Orchard or Cerner’s code program can facilitate smoother integration and exposure to health systems. For hospital IT teams implementing new apps, prioritize those that work with your current workflows (e.g. single sign-on with the EHR, ability to write data back to the patient record). Involvement of clinical end-users in selection and testing can ensure the app augments rather than disrupts their routine. Integration also extends to wearables and devices: ensure your patient apps can ingest data from the major consumer wearables (Apple HealthKit, Google Fit, etc.) if relevant, so patients don’t have to manually enter data that already exists elsewhere.
- Address the “Iron Triangle” of Requirements: The AMA found that physicians evaluate digital tools based on certain must-haves: Will it work (be effective)? Will I be reimbursed? Will I be liable? Will it fit into my practice?. Startups should keep these in mind when designing solutions and go-to-market strategies:
- Clinical effectiveness (we addressed above with evidence).
- Reimbursement/payment: If you expect clinicians to use or prescribe your app, consider how it aligns with their revenue streams. For example, does it help bill for remote monitoring codes? Can it be reimbursed through new digital health payment models? Alternatively, if selling to consumers, ensure pricing is reasonable or find a payer/employer subsidy model.
- Liability: Providers worry whether using an app could expose them to malpractice risk. To alleviate this, have clear disclaimers on what the app does and doesn’t do, incorporate clinical oversight (if needed) rather than fully replacing it, and obtain regulatory approvals for high-risk functions. Professional liability insurers are increasingly covering telehealth and digital tools, but you should clarify that your solution is intended to assist, not replace, clinical judgment (unless it’s a regulated autonomous therapeutic).
- Workflow fit: Again, integration and user-centered design will determine if the app actually gets used day-to-day.
- Focus on Interdisciplinary Collaboration: Healthcare is complex and building successful apps requires collaboration between technologists, healthcare professionals, and often patients. Startups should have clinicians (doctors, nurses, pharmacists relevant to your domain) involved from the concept stage through testing and iteration. Their insights will ensure the product is solving a real problem and is clinically sound. Similarly, hospital leaders implementing apps should involve not just IT, but also clinical champions and patient representatives in the selection process. An engaged clinician champion can help drive adoption among peers (“physician-to-physician” influence is powerful). Many failed health apps learned too late that building with the end-users, not just for them, is crucial.
- Plan for Change Management and Training: Hospitals rolling out a new mobile platform should not underestimate the need for training and support. Provide hands-on workshops for staff, easy how-to guides, and enlist “super-user” clinicians who can coach others. Address concerns openly – for instance, some nurses might fear a mobile app will monitor their performance; reassure how it will actually reduce their paperwork or enhance patient care. For patient-facing apps, consider providing digital literacy support or pairing the app with human coaches initially to on-board patients (studies show human coaching plus app yields better adherence than app alone). Essentially, treat a mobile health initiative as a change in care delivery, not just a software install.
- Measure, Improve, and Showcase Results: Use data analytics to monitor how the app is being used and its impact. Key metrics might include engagement (e.g. logins per week), clinical outcomes (e.g. reduction in HbA1c, hospitalizations), and patient or staff satisfaction scores. Share these results with stakeholders – e.g. if a hospital’s app reduces readmissions by 15%, that should be publicized internally and externally. For startups, having ROI case studies or improved outcome statistics will greatly help in marketing to providers and payers. It also allows iterative improvement of the product: if data shows a drop-off in usage after 1 month, you can investigate why (maybe users need more fresh content or follow-up reminders at that stage).
- Embrace Interoperability and Data Portability Ethically: Strategically, aligning with the broader move towards patient-centered interoperability can future-proof your app. Regulations like the ONC’s information blocking rule in the U.S. push for giving patients control of their data via APIs. If your solution can plug into these patient-authorized data flows (for example, enabling a user to import their hospital records into your chronic care app), it adds value to the user and strengthens your app’s utility. However, with that data comes responsibility – avoid the temptation to hoard data for competitive advantage or, worse, sell it inappropriately. Given rising awareness of data ethics, startups that position themselves as trustworthy stewards of patient data will have a competitive edge. Being transparent and even exceeding basic compliance (like adopting a privacy-first stance akin to Apple’s, which markets itself on data protection) can be a selling point.
- Think Global and Inclusive: Finally, consider the global and diverse context of healthcare. If you’re targeting emerging markets, strategies might differ (for instance, SMS-based apps or lightweight Android apps might be needed for areas with limited internet). Many countries are leapfrogging with mobile health to reach rural populations – pilots with simple maternal health SMS reminders by WHO showed improved prenatal care attendance, for example. Designing apps to work offline or in low-bandwidth conditions can open up new user bases. Also, be mindful of health disparities – ensure your app works for people with disabilities (compatibility with screen readers for the visually impaired, etc.) and is culturally sensitive. Healthcare mobile apps have the power to democratize access, but only if inclusivity is baked in.
By following these strategies, both startups and healthcare organizations can better navigate the digital health revolution. The mobile apps in healthcare industry are here to stay, but success requires going beyond the technology – it demands understanding human needs, earning trust, and integrating with the complex healthcare ecosystem. Those who get it right are poised to lead in an era where digital innovation and compassionate care go hand in hand.
Conclusion

Mobile health apps are catalyzing a shift toward more patient-centered, efficient, and proactive healthcare on a global scale. From a patient using an app to reverse diabetes, to a nurse triaging via secure chat, to AI algorithms silently monitoring heart rhythms through a smartwatch – these scenarios were the stuff of imagination a generation ago and are now increasingly routine. The benefits of mobile apps in healthcare – greater access, engagement, and data-driven care – have been clearly demonstrated, especially in recent years. Yet realizing their full potential requires surmounting adoption barriers and vigilantly safeguarding privacy and quality.
For healthcare providers, healthtech startups, and IT leaders, the mandate is to harness these digital tools thoughtfully: pick or build solutions that truly meet user needs, integrate them into care delivery, and continuously refine them with feedback and evidence. What are mobile health applications in the end? Not just software, but enablers of better patient care and health outcomes. By keeping the focus on patients’ and providers’ needs – and upholding the principles of trust, accessibility, and interoperability – healthcare mobile apps will continue to mature from novel gadgets into indispensable instruments of healing across the world.
Through collaborative efforts and innovation, mobile technology can help achieve the holy grail of healthcare: higher quality at lower cost, and health for people wherever they are. The organizations and innovators that lead in this space will undoubtedly drive the healthcare apps benefits forward – improving lives one download at a time.
Partner with Sosene: Future-Proof Your Healthcare App
Ready to revolutionize patient care with smart, scalable, and secure technology?
At Sosene, we help healthcare providers and healthtech innovators design, build, and scale advanced mobile applications—from telehealth platforms to AI-powered diagnostics and HIPAA-compliant patient portals.
FAQs
What are mobile health applications?
Mobile health applications (also known as healthcare mobile apps) are downloadable software for smartphones or tablets designed for use in healthcare by individuals or providers. They help users manage various health-related tasks such as tracking vital signs, scheduling doctor appointments, accessing medical records, or even conducting virtual consultations, bringing healthcare services conveniently into the digital realm.
What are the benefits of mobile apps in healthcare?
Mobile apps in healthcare provide convenient access to medical services and information anytime, anywhere. These tools let patients schedule appointments, receive medication reminders, access test results, and even consult doctors remotely, making it easier to follow care plans and communicate with providers. By improving engagement and communication, healthcare apps ultimately lead to higher patient satisfaction and better health outcomes.
How are mobile apps used in the healthcare industry?
In the healthcare industry, mobile apps are used by both patients and providers to enhance various aspects of care. Patients use health apps to monitor their wellness, schedule appointments, access personal health records, and even attend virtual telehealth visits, making care more accessible and efficient. Healthcare professionals also utilize mobile apps to review patient data, send appointment or medication reminders, and remotely monitor patients’ conditions for better ongoing care management.
How do healthcare mobile apps improve patient care?
Healthcare mobile apps improve patient care by making healthcare more accessible and patient-centered. These apps provide tools like medication reminders, educational resources, and instant communication with providers, which help patients stay on track with treatments and get timely medical advice when needed. By empowering patients to actively participate in their.




